Share:
Hello all!
So far with respect to practical seating considerations, I have written about pelvic obliquity, posterior pelvic tilt and anterior pelvic tilt. This month, I would like to focus on practical seating considerations for a client who presents with a pelvic rotation.
With pelvic rotation, one ASIS is positioned more forward relative to the other ASIS. (Please refer to the graphics below.)
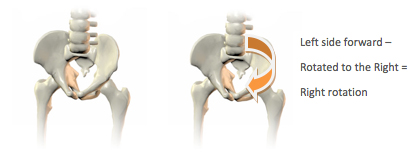
There are both clinical and technical reasons why a client may present with a pelvic rotation. Clinical reasons include: asymmetrical muscle tone (in the trunk and/or lower extremities); asymmetrical hip flexion; leg length discrepancy; and limited range of motion in hip abduction and/or adduction. Technical reasons for a client presenting with a pelvic rotation while sitting in his/her wheelchair include: the trunk not being supported; the back support not supporting the posterior pelvis; the seat to floor height being too high for foot propulsion; the seat and/or backrest contours being too narrow; and the wheelchair being set up incorrectly for hand propulsion.
As I have said in previous articles, it is only by taking the client out of the wheelchair and completing a thorough hands-on assessment that we can understand the cause(s) of a presenting posture. We need to understand the cause of the presenting posture and whether or not the posture is fixed or flexible in order to know what generic product parameters are required for the client's seating needs.
Imagine sitting with a significant pelvic rotation. If you can, go ahead and assume this posture while you are reading this. Are you now presenting with a windswept posture? Where are your feet positioned? Where is your back making contact with the back of your chair?
Now let's imagine that this is a fixed posture and we are seating a client with a fixed pelvic rotation. For a client sitting in a wheelchair, often the temptation is to try to separate the feet so that each foot is on a separate footrest and the feet are kept in position through the use of a foot strap. Medial thigh support may be added to the cushion to separate the legs, but is this really the best solution for a client with a fixed pelvic rotation? In the scenario I have just painted, we are not respecting the client's presenting posture.
Sharon Pratt, a physiotherapist and the Director of Education for Sunrise Medical US, has a wonderful saying: "Seating cannot sprinkle magic, perform surgery or administer medication." In the case of a client presenting with a fixed pelvic rotation, the seating and wheelchair configuration will have to accommodate the presenting posture. This may mean that a modified footplate has to be affixed to one hanger to accommodate the positioning of both feet. It may also mean that we have to provide education to care givers and others that just because there are two hangers on a wheelchair does not mean that each foot must be on a separate footrest for that particular client. The asymmetrical fixed posture must be respected with asymmetrical seating and positioning.
We also need to maximize the seated footprint. This means that we are ensuring that the surface contact area is maximized for both the cushion and the back rest for the client. This may mean adding components to a backrest to ensure the surface contact area is maximized when the client is sitting in an optimal position.
Something else that we must consider when seating a client with a fixed pelvic rotation and a windswept deformity is where is the point of the maximum width. It is this measurement that we must take when considering the overall width of the wheelchair to accommodate for the fixed windswept posture. For example, for a client with a fixed right rotation and windswept deformity, we need to consider the width between the left hip and the right knee when determining overall width requirements in a wheelchair.
I mentioned earlier that one of the clinical reasons that a client may present with a pelvic rotation is leg length discrepancy. If the cushion does not accommodate for a leg length discrepancy through a modification for the shorter leg, the client will be forced to rotate his/her pelvis to allow both knees to meet the edge of the cushion.
Similarly, if the cushion does not accommodate asymmetrical hip flexion, the client may rotate his/her pelvis to allow the hip with limited flexion to maintain a sitting position. Try it for yourself! Sit with our right hip at 90 degrees and your left hip at 75 degrees. What do you find happening to your pelvis? In this case, the cushion will need to accommodate the asymmetrical hip flexion to optimize the positioning of the pelvis.
Asymmetrical fixed postures and positions require asymmetrical solutions! We need to ensure that a full hands-on assessment is completed in order to determine the cause of a presenting posture so that the correct solution can be found for an individual client.