Share:
Hello all!
In last month's article, I wrote more on the practical seating considerations for posterior pelvic tilt. This month, I would like to focus on practical seating considerations for a client who presents with an anterior pelvic tilt.
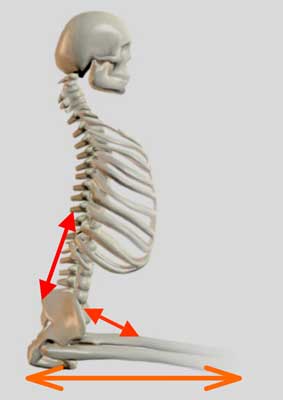
With an anterior pelvic tilt, the ASIS (anterior superior iliac spine) are lower than the PSIS (posterior superior iliac spine). See the graphic below.

When the PSIS are higher than the ASIS, we see an increase in the lumbar lordosis and a decrease in the hip angle. (Please refer to the figure below.)
Some of the clinical issues associated with anterior pelvic tilt include tight hip flexors tight quadriceps, tightened spinal extensors, weakened abdominal muscles, obesity, and increased lumbar lordosis.
There are also technical issues which may cause a client to present with an anterior pelvic tilt when sitting in his/her wheelchair. These include: excessive lumbar contour in the back rest; back support too vertical for the client, causing the client to lean forward; and having an anterior slope on the seat of the wheelchair.
It is only by taking the client out of the wheelchair and completing a thorough hands-on evaluation that we can understand the client's range of motion and flexibility available in the pelvis-spine and in the pelvis-hip joints. Using this information, we have a better understanding of the client's presenting posture and whether the client has a fixed or flexible anterior pelvic tilt.
In addressing the seating needs of a client who presents with an anterior pelvic tilt, we have to be cognizant of addressing the cause(s) of the posture, rather than providing a bandage solution. What do I mean by this? Well, often when a client presents with an anterior pelvic tilt, as the day progresses and the client fatigues, the client may lean more forward in his/her wheelchair, trying to gain more support through surfaces in front of the client, such as a lap tray. A bandage solution to this is to reach for a chest harness to try to pull the client back into an upright posture, but what we may find is that the chest harness does not work adequately to hold up fatigued muscles, and the client leans into the harness when fatigued. To truly address the cause of the forward leaning often associated with anterior pelvic tilt, we have to determine the cause of the presenting anterior pelvic tilt and address this with seating and wheelchair configuration choices.
We need to ensure that we are maximizing the client's "footprint" as he/she is seated. Maximizing the client's footprint means that the surface area contact is optimized on the areas on which the client can take load. This will include the cushion, footplates, backrest, headrest (if applicable), and arm rests/lap tray (if the client does not use his/her upper extremities for functional mobility). We may consider the use of a positioning belt to help maintain the pelvis in a neutral position (if the anterior pelvic tilt is flexible and if the client can tolerate correction). We may need to consider tilt in space to aid with positioning. It is only after we have looked at the cause(s) of the anterior pelvic tilt and have maximized the client's seated footprint through other choices that we would consider a chest harness.
Let's take a closer look at the importance of proper set-up of the footplates for a client who sits with an anterior pelvic tilt.
When a client sits with an anterior pelvic tilt, we often see the knees positioned at 90 degrees or less. In fact, how many times do we see the client sitting with their feet positioned on top of the heel loops or even behind the footplates? It is only by taking the client out of his/her current seating system and doing a thorough hands-on evaluation that we can determine the required hanger and footplate angles for a particular client. It may be that we need to position the footplates like either of the two figures below to accommodate the client's positioning needs.
Let me give you an example that illustrates the importance of footplates to which you might be able to relate. Have you ever sat on a bar stool that was missing the bottom rung? (If you have not, try to imagine what it would be like.) If you were to reach forward without having a stable base of support for your feet, you would find that you could not reach very far... or you might find that you try to wrap your legs around the bar stool to give yourself support so that you can try to reach for that nice, cold drink! We need proximal stability for distal function. By maximizing the seated footprint for a client, including through the footplates, we are providing stability to allow optimal function.