Share:
Hello all!
Last month's article gave us an overview of pressure sores, staging of pressure sores, factors associated with pressure sores and some prevention strategies. This month, I would like to look at how seating can assist in the prevention of skin breakdown and pressure ulcers.
Before we think about seating and skin protection, let's first think just about sitting. When we are sitting, the lowest point on the pelvis is the ischial tuberosities. In the left figure below, the ischial tuberosities are highlighted by the blue circles and in the right figure below, the ischials are indicated by the small arrows.
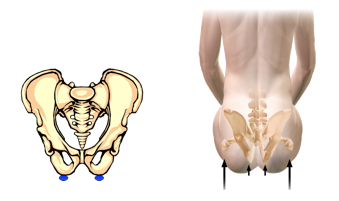
An interesting reaction happens to our bodies when we sit. Our bodies react with gravity and the fat and muscle directly beneath the ischial tuberosities slowly move away from the point below the ischia, causing the ischial tuberosities to be closer to the skin. As we sit, this condition continues. After time, the pressure experienced by the skin under the ischial tuberosities causes the capillaries to close, resulting in the skin cells beginning to die due to lack of oxygen and nutrients. This can occur in as little as 10 to 15 minutes if there has been no weight shifting.1 As we continue to sit, the soft tissue continues to spread and the bony contact area increases. The trochanters may also begin to experience pressure. Discomfort will occur in about 30 minutes.1 (See the graphic to the right, above, that shows the relative position of the ischial tuberosities to the trochanters. The trochanters are highlighted by the larger arrows.) This reaction of our bodies with gravity explains why when we are seated on a hard chair or a thin cushion for a period of time we begin to experience discomfort (assuming we are sensate) and find ourselves shifting and changing position to relieve the pressure.
Now let's think about wheelchair cushions. Wheelchair cushions function to address comfort (i.e. increase sitting tolerance), provide support, and allow for pressure reduction. The design of wheelchair cushions can also address shear reduction and heat and moisture dissipation, which are also factors in skin protection. That being said, it is important to remember that we cannot rely solely on the cushion to prevent the formation of pressure ulcers.2 (Refer back to the strategies to prevent pressure ulcer formation listed in last month's article on Pressure Sores and Skin Protection.) In addition, it is important to remember that one type of cushion will not work for everyone.2
This month, let's think about pressure reduction. How can seating help to reduce pressure? One way is through maximizing the surface contact area. Since the formula for pressure is equal to force divided by area, if we maximize the seated surface area, the pressure over the entire area is lower.3 We should consider not only the contact area of the cushion, but also of the back rest. That is not to say that we should provide all clients will tall backrests in order to maximize surface contact area with the back support as a tall backrest can limit function for some clients. What is meant is that the contact area between the client's back and his/her backrest, whatever height of backrest is required by the client for optimal support and function, is maximized. The use of shape, such as lumbar support, may help to maximize surface contact area in the backrest.
We also have to think about minimizing peak pressures, which occur at the bony prominences, such as the ischial tuberosities. Visually, we may see an area of redness at a bony prominence on a client, and this typically indicates an area of peak pressure experienced by the client. How can cushions minimize peak pressures? Manufacturers use materials and product design in order to protect the bony prominences. Different materials react differently with the body and offer various levels of skin protection based on their properties. Product design also is used to redistribute load and offer protection to the bony prominences.
There is a lot to consider in terms of skin protection through seating. Future articles will address the various materials that manufacturers use in cushion design and their impact on pressure and shear reduction; how product design is used to redistribute load; and considerations for heat and moisture dissipation through seating.
Resources
- Semble, JA. (1994). The Biomechanical Relationship of seat design to human anatomy. In R. Lueder & K. Noro (Eds.), Hard Facts about Soft Machines. The Ergonomics of Seating (pp. 221-230). Encino, CA: Taylor & Francis.
- Batavia, M. (2010). The Wheelchair Evaluation. A Clinician's Guide. (2nd ed.). Sudbury, MA: Jones and Bartlett Publishers.
- Cooper, R. (1998). Wheelchair Selection and Configuration. New York: Demos Medical Publishing.