Share:
Hello all!
Recently, I received an email question through my blog from an occupational therapist and her question struck me as a really interesting example of how product design can influence skin protection in a particular clinical scenario. With the therapist's consent, I will share a synopsis of her question to me and my response. (Please note that some of the details regarding the client have been altered to ensure client privacy.)
The therapist described a client who was a bilateral, above-knee amputee. The therapist reported that comfort and pressure were becoming issues for this client, who was losing muscle mass in the glutes with age. On pressure mapping, there was increased pressure at the ITs and also at the coccyx when the client sat in a posterior pelvic tilt; there was no loading through the thighs. The therapist reported that the client sat on a cushion that was contoured foam with gel.
When I read this question, I immediately thought that the cushion design and the level of "gel" or fluid in the well would have a significant effect on redistribution of load to the thighs and on skin protection. Although the therapist did not mention the actual model of cushion her client used, I wondered if the cushion design was one in which the entire pelvis sits in the well of the cushion (i.e. the well is larger than the width of an adult pelvis) and the pelvis "floats" in a pressure relieving material.
I advised the therapist if the design of the cushion was one in which the entire pelvis sits in a pressure relieving material, such as a fluid, she may want to consider having a cushion modified to include an overfill of the fluid, given the described atrophy of the glutes. Fluid in the well of a cushion can be thought of as being a replacement for a client's tissue, so a client with very little tissue would require more fluid in a cushion than a client with excess tissue would require. With a greater amount of fluid in the well, the client may sit higher on the well which could allow the load to be redistributed to the femurs (rather than sinking deep into the well causing bottoming out and increased hip flexion which means that the thighs cannot be loaded). In my mind, I had pictured the therapist's client sitting somewhat like this (where the dotted lines represent the femurs), with there being insufficient fluid for that particular client's shape to support the buttocks at the correct height to allow loading of the femurs through the base of the cushion, even though the tissue of the thighs may have been making contact with the cushion:
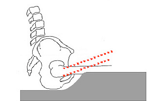
I advised the therapist that another solution would be to consider a cushion in which the shape of the well is such that the trochanters are supported on the sloped edge of the well. This type of design allows for the ITs to be immersed into the pressure relieving fluid in the well, while the load is redistributed to the trochanters and the femurs. (I reminded the therapist that the trochanters can take load as long as a client has not had hip surgery or hip dislocation or skin breakdown at the trochanters.) With the proper sized well, the under surface of the trochanters are supported, so the client doesn't sink too far into the well, which then promotes the load being redistributed to the trochanters and the femurs. Once again, with this type of cushion, overfill of the fluid can be ordered, if it is required for a client with atrophy of the glutes.
From the therapist's description that there was increased pressure on the coccyx on pressuring mapping when the client sat in a posterior pelvic tilt, I told the therapist I assumed the client had a flexible posterior pelvic tilt which the client could self-correct. I then asked the therapist some questions to prod her thinking. (She may have thought of all this already, but this information was not included in her question to me.) I asked if the client had a firm back support that starts at, or just below, the level of the PSIS? This is needed to help position the client's pelvis as optimally as possible for the client. I reminded the therapist that a cushion will not function the way it was intended to function if there is not adequate support at the posterior pelvis through the back rest. I asked if the backrest was pressure mapped in addition to the cushion to ensure that the client was taking load through her back support as well, and that the surface contact area was maximized. I explained that I have seen pressure mapping where, although there was a back rest, the client was taking very little load through the back rest, so all of the client's load was distributed through the cushion, resulting in peak pressures at bony prominences.
Here is an example of the difference in pressure mapping on the cushion when the backrest is not taking load versus when the backrest is taking load (the pressure mapping above the grey line is the back support and the area below the grey line is the cushion):
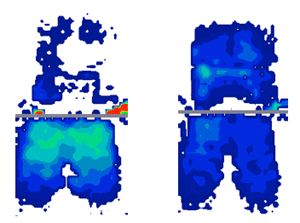
Notice the effect on the pressure mapping of the cushion when the back rest has increased loading, as seen in the picture to the right, which shows a more even pressure distribution.
I reminded the therapist that if the client continues to sit in a posterior pelvic tilt, despite adequate posterior pelvic support, she should think about the orientation of the ITs in relation to the anterior wall of the well of the cushion. For some clients, the ITs may come too close to the anterior aspect of the well, causing increased pressure at the ITs. To solve this issue, a modification to the foam base to move the well forward can be requested (e.g. move well 1 inch or 2 inches forward and have a corresponding 1 inch or 2 inches of foam added to the back of the well.)
I also reminded the therapist that when using a cushion with fluid, maintenance of the cushion will always be required. Maintenance involves kneading the fluid to ensure that the fluid is properly distributed within the well so that bottoming out does not occur. If a client slides into posterior pelvic tilt frequently, the required frequency of kneading may be increased as the ischials may displace the fluid with this movement. I added that even if the fluid inserts are segmented to minimize fluid migration, kneading still is required.
I summarized by saying: So, in a nutshell, when you tell me that your client, who is a bilateral amputee, is not taking load through the femurs, and has increased pressure at the ITs and sometimes the coccyx when the client sits in posterior pelvic tilt, my immediate thought goes to shape and depth of the cushion well so that the load can be redirected to the femurs (and possibly the trochanters). I also think about the amount of fluid available in the well to ensure it is sufficient to envelop the client's buttocks for full immersion and more even pressure distribution. In addition, I think about how the back support works with the cushion to redistribute load over a larger surface contact area.
So, I hope by sharing my answer to this clinical question you can see how product design can have an impact on redistribution of load and skin protection. My thanks go to the therapist for sending me this interesting question and for letting me share her question and my answer with all of you!